Specific Thyroid Surgery Procedures Dictate Later Risk of Hypoparathyroidism
Written by |
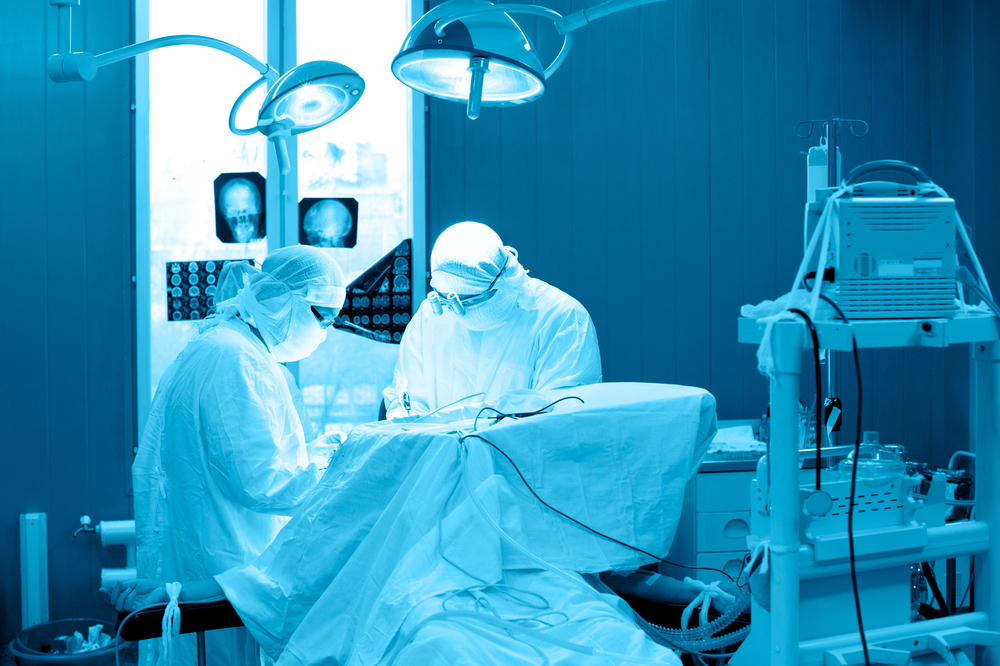
The specific surgical procedures used when patients undergo thyroid surgery — known as thyroidectomy — dictate the risks they have of developing hypoparathyroidism and other complications, a study found.
Because this type of surgery is associated with a high risk of complications and requires specialized care, it should only be performed by experienced surgeons, the investigators said.
The study, “Complications after medullary thyroid carcinoma surgery: multicentre study of the SQRTPA and EUROCRINE databases,” conducted by researchers in Sweden and Germany, was published in the British Journal of Surgery.
Thyroid removal is the standard procedure for patients with medullary thyroid carcinoma (MTC), a form of thyroid cancer that is estimated to affect nearly 0.5 per 100,000 people. Yet, the scientists said that clinicians should first weigh its benefits in treating cancer against the risk of surgical complications.
Hypoparathyroidism and RLN palsy were considered at least temporary in the cases in which patients were still on medication at a second follow-up visit or at a first follow-up appointment without subsequent data. Statistical analyses were used to determine potential risk factors for surgical complications that were at least temporary.
Among the patients analyzed, 170 (26.2%) developed hypoparathyroidism. In turn, among the 451 patients who underwent laryngoscopy after surgery, 62 (13.7%) had at least temporary RLN palsy. A total of 17 people (2.6%) experienced bleeding that required reoperation after having thyroid surgery.




