Clinicians Should Consider Hypoparathyroidism When Symptoms Suggest Brain Calcification, Case Study Says
Clinicians should consider the possibility of hypoparathyroidism in patients with chronic low levels of calcium, recurrent twitching of hands or feet, and even epileptic-like psychiatric symptoms to ensure early diagnosis and treatment, a case study reports.
The study, “Hypoparathyroidism with Fahr’s syndrome: A case report and review of the literature,” was published in the World Journal of Clinical Cases.
Hypoparathyroidism is caused by a deficiency in the parathyroid hormone (PTH) and is characterized by low levels of calcium, or hypocalcemia, and high levels of phosphorus (hyperphosphatemia) in the blood.
This disorder is often associated with abnormal deposits of calcium (calcifications) in the basal ganglia, a collection of small structures deep in the brain that play important roles in movement control. Such brain calcification in these patients is called Fahr’s syndrome, owing to its similar manifestations with a rare genetic disorder called Fahr’s disease.
Both are characterized by progressive deterioration of mental abilities, slurred speech, and loss of motor skills. This can be accompanied by uncontrollable spasmodic movements (chorea), twisting movements of the hands and feet known as tetany, muscle cramps, and seizures.
But while Fahr’s disease is an illness on its own, Fahr’s syndrome develops as a consequence of other conditions, most commonly hypoparathyroidism.
Researchers described one such case in a 62-year-old Chinese man, who had been experiencing repeated twitching of both hands over the past decade. He had been diagnosed earlier with hypocalcemia at a primary hospital, but hadn’t undergone thorough exams so had not been given a definitive diagnosis.
The patient was prescribed a calcium supplement at the time, but his compliance was poor and symptoms returned.
He was admitted to the emergency department of the People’s Hospital of Yuxi City, in China, complaining of slow response and speech difficulties.
On medical examinations, he had a positive Chvostek sign, which is a clinical sign of nerve hyperexcitability (tetany) and marker of low calcium levels. He had no history of neck surgery or radiation, which can be causes of hypoparathyroidism.
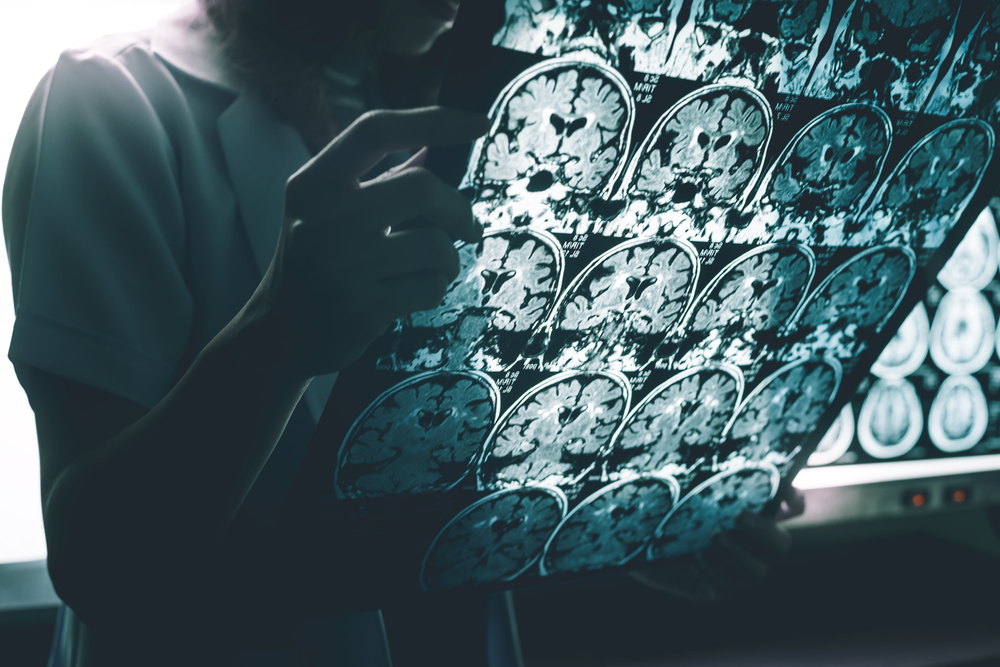
However, laboratory tests confirmed he had hypocalcemia, hyperphosphatemia, and low PTH levels. Brain imaging by computed tomography scans revealed basal ganglia calcification. Based on these signs, the patient was diagnosed with Fahr’s syndrome due to hypoparathyroidism.
At the hospital, he was treated with continuous drip infusions of calcium gluconate for rapid relief of symptoms. Treatment followed with oral calcium carbonate (another form of calcium supplementation) and activated vitamin D (calcitriol), which he continued at home.
Overall, this case calls attention to the importance of standardized treatment and follow-up in patients with hypoparathyroidism, the researchers said.
“[F]or patients with long-term hypocalcemia, recurrent tetany, or even epileptic-like psychiatric symptoms, clinicians should associate with the possibility of hypoparathyroidism in order to make early diagnosis and treatment,” they wrote.
The team recommended that clinicians “first consider the possibility of hypoparathyroidism when looking for the cause of basal ganglia calcification” and determine blood calcium, phosphorus, and PTH levels in all individuals with such calcification to exclude hypoparathyroidism.
Because hypoparathyroidism is often accompanied by other complications and comorbidities, it “is important for clinicians, especially endocrinologists, to understand the clinical manifestations, diagnosis, and treatment of the disease,” the investigators said.